FASCIAPUNCTURE® CLINICAL THINKING
When Rest Feels Unsafe
The Nervous System Behind Burnout
Burnout is not always a failure to rest. Sometimes it is the loss of the capacity to feel safe while resting.
Rest is not always accessible. In a protected system, stillness may first be interpreted as threat.
A CLINICAL REFLECTION ON BURNOUT
Some People Are Exhausted Because Their Nervous System No Longer Knows How to Rest
One of the most misunderstood aspects of burnout is this:
Some people are not exhausted because they work too much. They are exhausted because their nervous system no longer knows how to rest.
In clinical practice, I often hear:
- “When I slow down, I feel worse.”
- “If I stop, anxiety rises.”
- “Rest makes me uncomfortable.”
This is not a psychological weakness. It is a physiological state.
Sometimes rest first reveals alarm.
BURNOUT IS NOT JUST FATIGUE
A Nervous System Locked in Survival Mode
Burnout is often described as tiredness, lack of motivation, or emotional depletion.
But beneath these labels lies something more precise:
When the sympathetic system stays dominant for too long, rest is no longer perceived as safe.
Silence becomes threatening. Stillness feels like loss of control.
Movement, activity, and intensity become ways to regulate anxiety — not expressions of vitality.
WHEN REST TRIGGERS ALARM
For a Dysregulated System, Rest Allows What Was Hidden to Surface
For a regulated system, rest allows recovery.
For a dysregulated one, rest can trigger:
- inner agitation
- racing thoughts
- sudden emotional waves
- bodily discomfort
- a sense of emptiness or danger
In these cases, “doing nothing” is not soothing. It removes the last coping strategy the system has.
This is why telling someone in burnout to “just rest” often fails.
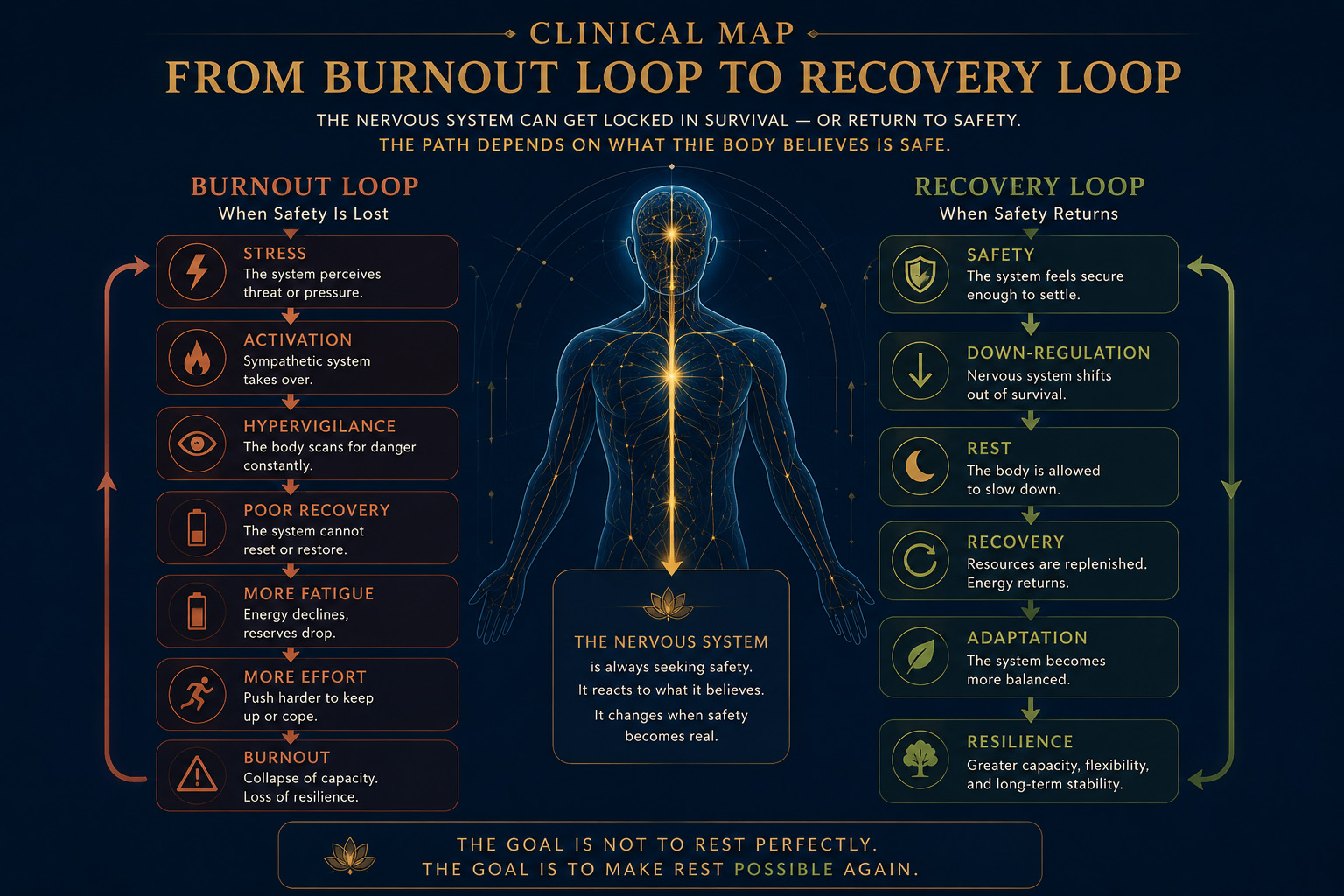
CLINICAL MAP
From Burnout Loop to Recovery Loop
When Safety Is Lost
Stress
↓
Activation
↓
Hypervigilance
↓
Poor Recovery
↓
More Fatigue
↓
More Effort
↓
Burnout
When Safety Returns
Safety
↓
Down-Regulation
↓
Rest
↓
Recovery
↓
Adaptation
↓
Resilience
YIN CANNOT BE FORCED
Recovery Begins Not with Stopping, but with Reducing Threat
In traditional Chinese medicine, Yin represents restoration, grounding, internal regulation, and the capacity to settle.
But Yin cannot be imposed by will.
A system that has lived too long in Yang does not enter Yin suddenly. It must be guided there.
but with reducing threat.
RELATED CLINICAL PATTERNS
This reflection belongs to the wider Clinical Map
Global Protective State
When the body remains organized around vigilance, protection, and long-term survival adaptation.
SYSTEMIC REGULATIONAutonomic Dysregulation
When activation and recovery no longer alternate naturally, and rest becomes difficult to access.
RECOVERY PATTERNSystem Exhaustion
When the body is tired but still unable to descend into true recovery.
BREATHING AXISDiaphragm Restriction
When breathing remains high, guarded, or unable to support down-regulation.
A CLINICAL PERSPECTIVE
Help the Nervous System Rediscover That Rest Can Be Safe
My role as a practitioner is not to push patients into stillness.
It is to help their nervous system rediscover that rest can be safe.
This happens gradually:
- by slowing the internal rhythm
- by creating zones of regulation
- by restoring trust inside the body
Only then does rest become nourishing instead of destabilizing.
CLINICAL PRINCIPLE
Burnout Is Not a Failure to Rest
Burnout is a loss of the capacity to feel safe while resting.
And that capacity can be rebuilt.
Not through force. But through rhythm.
Stillness is interpreted as threat.
WHY INTERVENTION IS POSSIBLE
Down-Regulation Without Activating Defensive Responses
Fasciapuncture® does not ask the nervous system to “feel safe” through suggestion alone.
It accesses peripheral neuro-fascial entry zones where neural density and fascial continuity allow down-regulation without activating defensive responses.
This makes it possible to intervene before safety is consciously available, using anatomy rather than psychology as the entry point.
It is reintroduced through regulation.
FASCIAPUNCTURE® TRAINING
These Principles Become Clinical Skills
- precise identification of neuro-fascial entry zones
- distinction between regulatory, destabilizing, and non-indicated areas
- clinical decision-making based on system state rather than symptoms
- recognition of when stillness is therapeutic and when it becomes threatening
FINAL REFLECTION
Rest Becomes Recovery Only When the Body Feels Safe Enough to Receive It
Burnout is not simply exhaustion.
It is often the body’s inability to return safely from activation.
When rest feels unsafe, recovery cannot be forced. It must be rebuilt through regulation, trust, and rhythm.
Threat is.
CONTINUE EXPLORING
Learn to read burnout through the nervous system
Fasciapuncture® reads burnout not only as fatigue, but as a loss of regulatory access — a state where the body needs safety before it can truly recover.

