Introduction
In clinical practice, it is common to encounter patients who describe a puzzling combination of symptoms.
They report anxiety, fragmented sleep, and diffuse physical pain that appears to worsen during periods of emotional stress. Medical examinations often fail to reveal structural abnormalities, leaving both the patient and practitioner uncertain about the origin of the symptoms.
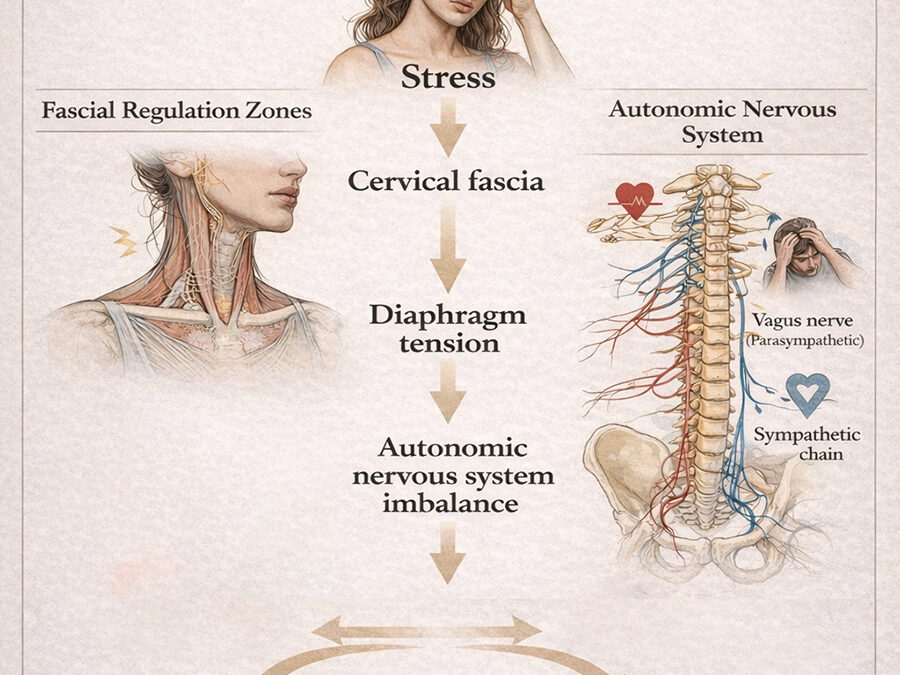
This article presents a clinical observation illustrating how emotional stress may manifest physically through the fascial and autonomic systems.
Understanding this relationship can help clinicians interpret symptoms that otherwise appear unrelated.
Clinical Observation
A 35-year-old woman consulted for recurrent episodes of diffuse joint discomfort. The symptoms appeared intermittently and were clearly associated with periods of emotional stress.
Her primary complaints included:
-
Anxiety and mental tension
-
Frequent awakening between 1 and 3 a.m.
-
Episodes of generalized joint pain during stressful situations
-
Normal digestive function
The patient also reported hormonal suppression of menstruation through medication.
Although the joints themselves showed no structural pathology, palpatory examination revealed areas of increased fascial tension in several regulatory regions of the body.
These findings suggested that the symptoms were not primarily orthopedic in origin.
Fascia and Systemic Regulation
Fascia is increasingly recognized as a continuous connective network that surrounds and links muscles, organs, nerves, and vascular structures throughout the body.
Beyond its structural role, fascia participates in:
-
mechanical force transmission
-
sensory perception
-
autonomic regulation
Because of this integrative function, alterations in autonomic balance can influence fascial tone across the body.
Emotional stress activates the sympathetic nervous system, which may increase muscular and fascial tension. When this state persists, the fascial network can amplify sensory input, lowering the threshold at which stimuli are perceived as pain.
In such situations, discomfort may appear in multiple joints even though no structural damage is present.
Sleep Disturbance and Autonomic Activity
Night-time awakening between one and three in the morning is frequently associated with heightened autonomic arousal.
Rather than entering a stable restorative phase of sleep, the nervous system remains partially activated.
In many individuals, fascial tension around the thoracic region and diaphragm can influence respiratory rhythm and autonomic modulation. These subtle mechanical changes may contribute to the sleep disturbances observed in stress-related conditions.
Thus, sleep fragmentation and diffuse pain may share a common regulatory background.
Clinical Interpretation
From a fascia-oriented perspective, the patient’s symptoms can be understood as a systemic regulatory pattern rather than isolated local problems.
Emotional stress triggers autonomic activation.
Autonomic activation increases fascial tone.
Persistent fascial tension alters sensory processing.
As a result, physical discomfort emerges even in the absence of structural pathology.
This interpretation shifts the clinical focus from symptomatic structures to the regulatory networks that coordinate the body’s internal balance.
Clinical Perspective
Cases of stress-related diffuse pain are increasingly encountered in modern clinical practice.
Such presentations highlight the importance of considering the body as an integrated system rather than a collection of independent parts.
When the fascial network and autonomic regulation are viewed together, symptoms that once appeared unrelated—such as anxiety, sleep disturbance, and musculoskeletal pain—can often be understood within a coherent physiological framework.
Further research and clinical observation will continue to clarify the role of fascia in systemic regulation and sensory modulation.
Conclusion
Pain does not always originate where it is perceived.
In many situations, symptoms arise from broader regulatory changes within the body’s interconnected systems.
Recognizing the relationship between emotional stress, autonomic activity, and fascial tension may provide valuable insight into complex clinical presentations.
Such perspectives encourage a more integrative understanding of human physiology—one that considers both structural and regulatory dimensions of health.